Should hypermobile people do Yin Yoga?
By Bernie Clark, Revised December 6, 2019
Should hypermobile students do Yin Yoga? The question is actually much broader—should hypermobile students do yoga? The answer is “yes, no, maybe” – it depends! It depends upon what causes the hypermobility. We can generalize three causes of hypermobility:
 Enhanced ranges of motion due to an injury to a joint
Enhanced ranges of motion due to an injury to a joint- Enhanced ranges of motion due to a connective disease or disorder
- Enhanced ranges of motion due to skeletal variations.
Students who are hypermobile due to an injury to a joint should be careful of over-stressing that joint. It needs time to heal. This does not necessary mean that the joint should be immobilized, as that often leads to undesirable side effects, but care should be taken not to go to the joint’s end range of motion because that end range is only possible right now due to damage to the restraining connective tissues. A yoga practice now should work well within the tolerable ranges of motion and should lead to strengthening the joint, not lengthening it. Yin Yoga at this time is probably not a great idea.
Students who are hypermobile due to a connective tissue disorder, someone with Marfan syndrome or Ehlers Danlos Syndrome, have a genetic difference in the way their collagen is structured. It is very loose and can allow too much movement in a joint. These students should be very careful doing yoga in general, and that includes Yin Yoga. They do not need to work on increasing their range of motion but rather on building strength and stability in the joints. They can certainly try yoga, or even Yin Yoga, but only with great attention and with the intention of building strength in their tissues, not flexibility. They need to pay attention to how the practice affects them and how it feels—while they are in the postures, when they come out of the postures and over the next day or two. Through trial and error, through intention and attention, they will develop their own sensitivity to what works for them and what doesn’t. If they were to try Yin Yoga (perhaps to obtain the meditative, psycho-emotional or energetic benefits), shorter holds of 1 to 2 minutes to start would be recommended, and they should try to go only halfway to their edge, not to their end range of movement.
Students who are injured or who have connective tissue disorders are fortunately rare, maybe one in a thousand, but they are around. They do not always announce themselves to yoga teachers, but if you fit one of these categories, it is advisable to let your teacher know that you will be modifying the postures to suit your unique situation. As a teacher, please help to train the student to know how to listen to their body, start easy and go slow.
However, most people who are hypermobile are more flexible than the norm not because of an injury or condition, but due to the shape of their bones. What looks like a dangerous range of motion is actually quite normal and healthy, for them. They do not have to be brought back from their natural range of motion, although, like for every student, they should be guided to recognize when an end range has been reached and taught to not try to go past that point.
A caution that is appropriate for one hypermobile student may not be necessary for another. Many people are considered hypermobile. Estimates vary from less than 1% of the population to as much as 25%. [1] But, as we have just seen, the cause of the hypermobility has to be taken into consideration. One very mobile yoga student was told by her teacher, “You are too flexible for a Yin Yoga practice!” When asked why, she was told, “Putting any kind of stress on the ligaments, is unhealthy and unsafe.” She was, however, encouraged to continue her Ashtanga and Iyengar practices, which require far more ranges of motion that Yin Yoga does. Should she do Yin Yoga? Her intuition gave her a very different answer – she loved doing Yin Yoga along with her more active practices, but she was in a dilemma – who to believe? If the teacher had instead said, “Let’s see if we can determine why you are hypermobile and then decide on the best practice for you,” together the teacher and student would have been able to develop a practice specifically suited to this student’s unique requirements.
Hypermobility Syndrome
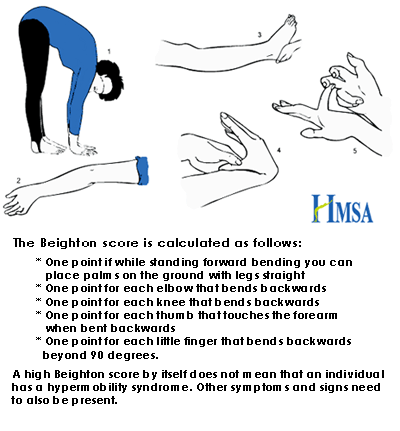
Often the overarching term used for very flexible people is hypermobility syndrome, or HMS. Sometimes the terms used are joint hypermobility syndrome (JHS) or generalized joint laxity (GJL). HMS is defined to be an abnormally large range of motion of one or more joints in the body. A clinical diagnosis of hypermobility can be done via several tests, such as the Beighton Hypermobility score, which measures several joints’ range of motion and includes the ability to place both hands on the floor with legs straight. [2] While many people have high scores in these tests, being diagnosed as hypermobility does not mean that you will ever have any problems because of your flexibility. Most hypermobile people are asymptomatic and suffer no ill from their large range of motion. However, for a small percentage of the population, being hypermobile does have definite negative consequences. These are the people in category 1 and 2 cited above, who have an injury or who may suffer Marfan Syndrome, Ehlers Danlos Syndrome (EDS), Osteogenesis Imperfecta or Sticklers Syndrome. Each of condition has its individual causes, symptoms and recommendations.
 The incidence of hypermobility is correlated with age and gender, and with ethnicity. Children have much more flexibility than adults and are more likely to be diagnoses as hypermobile, but most will grow out of it. This is partially due to the change in our bones as we mature. Thinner bones tend to allow for more range of motion than bigger bones. Women are up to 5 times more likely to be diagnosed with HMS than men. [3] Studies of various ethnicities show wide variations in occurrence of HMS.
The incidence of hypermobility is correlated with age and gender, and with ethnicity. Children have much more flexibility than adults and are more likely to be diagnoses as hypermobile, but most will grow out of it. This is partially due to the change in our bones as we mature. Thinner bones tend to allow for more range of motion than bigger bones. Women are up to 5 times more likely to be diagnosed with HMS than men. [3] Studies of various ethnicities show wide variations in occurrence of HMS.
The incidences of HMS due to underlying pathology or genetic causes are far rarer than generalized joint laxity. Ehlers Danlos Syndrome affects one in person in 2,500 to 5,000: it is a genetic connective tissue disorder that can cause problems in any connective tissue, which basically means everywhere: the fascia, muscles, bones, skin and even the organs. Marfan Syndrome is usually inherited, but not always, affecting 1 person in 5,000. Like EDS, it is a connective tissue problem and can create problems in the heart, blood vessels, lungs, eyes as well as in the bones and joints. People with genetically caused hypermobility may have symptoms of pain and fatigue, which are not so surprising, but other symptoms can include poor proprioception, balance and generalized anxiety. In extreme cases, these heritable disorders of the connective tissues can have life threatening complications and medical advice should be sought.
Advice for hypermobile students
One often given piece of advice to hypermobile people of any cause is to avoid holding postures that take the joints to their extreme ranges of motion. Examples can range from slouching in a chair to holding weight in one hip while standing on that leg. Certainly yoga would seem contraindicated for hypermobile people, but despite the warnings, most hypermobile people love to stretch and need to stretch! [4] Curiously, stiffness is a common complaint of many hypermobile people. As they age or suffer injury, they lose the range of motion they once had, and although they may still look very flexible, they are not normal for them. They crave stretching.
It is worthwhile to differentiate between stretching for health (which is okay for people in the third category listed at the beginning) and stretching to increase an already unstable, hypermobile range of motion (which would not be good for those in category 1 or 2). Authors of a book promoting therapies for hypermobility wrote that we must note the difference between, “stretching performed in order to regain and maintain muscle length, relieve muscle tension, or restore and maintain joint range, and stretching to increase an already hypermobile range of motion. It is good to stretch, but care is required. [Emphasis added.] Educating an individual about how they can stretch safely without overstretching into their hypermobile or more vulnerable areas will help develop better body awareness, a skill which can be used in the future to ensure safe exercising.” [5]
Yoga is not contraindicated and indeed can be a healthy adjunct to the exercises hypermobile people perform, with the caveat that sustained end of range movements are not recommended. Strength building is generally a good thing; it helps to promote stability. We can turn this understanding into a graph: figure 3 shows an N-shaped curve with health along the vertical axis and flexibility along the horizontal axis. If we have little flexibility, we are not very healthy. However, if we have too much flexibility, we are again at risk of poor health. However, we need flexibility! Where the middle of this curve is for you may be quite different from someone else, but our intention should be to come to the middle. If we are on the left side of the middle, we need to work on increasing mobility (stretching). If we are on the right side, we need to work on stability (strength). In both cases we want to seek our optimal range of motion to maximize health.
![]() Remember the warning: avoid sustained end of range motion. Now that we know yoga is okay for most hypermobile students, the question now comes back to – is Yin Yoga safe for hypermobile students? The question can be turned into – which style of yoga is most likely to take the student to her end range of motion? It turns out that the risk is often not Yin Yoga but the deeper postures of active practices like Iyengar and Ashtanga!
Remember the warning: avoid sustained end of range motion. Now that we know yoga is okay for most hypermobile students, the question now comes back to – is Yin Yoga safe for hypermobile students? The question can be turned into – which style of yoga is most likely to take the student to her end range of motion? It turns out that the risk is often not Yin Yoga but the deeper postures of active practices like Iyengar and Ashtanga!
The repertoire of Yin Yoga postures is quite small compared to the number of postures used in the more active forms of Hatha Yoga. The intention in Yin Yoga is to stress the connective tissues that surround and invest the muscles, joints, and organs. Connective tissue makes up our fascia, tendons, ligaments and joint capsules. These fabrics need stress to regain and maintain optimal health. If they are short, contracted and stiff, they need to be stressed to regain their natural ranges of motion. But the intention of Yin Yoga is not to become hypermobile. The practice in Yin Yoga is to guide a student to an edge, where there is a stress, but not to their ultimate depth in any posture. The student is encouraged to linger at the edge, but not seek greater depth. Time is more important than intensity. Indeed, there are only a couple of postures in Yin Yoga that will take a very flexible student anywhere near her end ranges of motion (Straddle and some Dragon variations). Compare the depth in postures from the Yin Yoga repertoire and the advanced asanas of Iyengar/Ashtanga practices:
- For flexion of the hips, which is deeper Caterpillar or Tittibhasana II?
- For external rotation at the hips, which is deeper Winged Dragon or Ekapadasirsasana?
- For extension of the spine, which is deeper Seal or Wheel?
- For flexion for the spine, which is deeper Butterfly or Suptakurmasana?



 We could go on and on: Yin Yoga’s Snail pose is not nearly a deep spinal flexion as Ashtanga’s Karnapidasana pose. In each instance, the Yin Yoga asana does not take a hypermobile student close to her end range of movement, but that can happen in the more active practices, which involves dynamic stresses of the joints at their extreme positions. Dropping back into the Wheel pose, a common Ashtanga practice, is not a great idea for someone who is hypermobile.
We could go on and on: Yin Yoga’s Snail pose is not nearly a deep spinal flexion as Ashtanga’s Karnapidasana pose. In each instance, the Yin Yoga asana does not take a hypermobile student close to her end range of movement, but that can happen in the more active practices, which involves dynamic stresses of the joints at their extreme positions. Dropping back into the Wheel pose, a common Ashtanga practice, is not a great idea for someone who is hypermobile.
Yin Yoga is safer than the deep postures found in advanced Iyengar and Ashtanga yoga. Yin Yoga will not come close to challenging hypermobile students at their end ranges of motion, but Yin Yoga will still apply an essential stress to the joints and other connective tissues. Remember – hypermobile people do need to stretch! Joints and ligaments need stress! Each student will have to determine for herself the optimal length of time to stay in the postures: remember, shorter holds are advisable in the beginning until the student can determine whether it is wise to stay longer in these postures. [6]
Many people are hypermobile and are asymptomatic: they live full, healthy lives with no problem and don’t need to be fixed or pampered. Others do need to take great care. The reality is, we cannot treat everyone the same. There is a spectrum of hypermobility and a variety of causes. The best a teacher can do is help students know where they are on this spectrum so that they can figure out for themselves what is appropriate.
The fear of going too far is real for hypermobile people, and the danger is real too. Depending upon the cause of the hypermobility, Yin Yoga can be a safe practice, one that does not challenge end ranges of motion, but one that does provide the stress hypermobile people crave and need. Yin Yoga does target the connective tissues, which is where pathology lies for people with genetic connective tissue disorders. However, for students who are hypermobile, not because of any condition or disease but because of the unique shape of their bones, there is no pathology preventing them from going to their natural, full range of motion. It is safe to go there.
Before starting any exercise practice, yoga or otherwise, it is wise to check with your health care provider to make sure this is a good idea. Do your research. If you are hypermobile and choose to do Yin Yoga, practice with attention and intention. Start easy – short holds at first of 1 to 2 minutes, only going halfway to your end range of motion, notice how you feel during and after the practice, work towards longer holds, but remember the intention is not enhanced range of motion; the intention is regain and maintain optimal health.
Footnotes:
- — See Scher DL1, Owens BD, Sturdivant RX, Wolf JM.: Incidence of joint hypermobility syndrome in a military population: impact of gender and race. Clin Orthop Relat Res. 2010 Jul;468(7):1790-5. doi: 10.1007/s11999-009-1182-2.
- — Beighton PH Horan F.: Orthopedic aspects of the Ehlers-Danlos syndrome. J Bone Joint Surg [Br]. 1969; 51: 444-453.
- — “Hypermobility syndrome is 1.1 times to 5.5 times more prevalent in women than in men.” Leslie N Russek: Examination and Treatment of a Patient With Hypermobility Syndrome in PHYS THER. 2000; 80:386-398.
- < — “An unpublished audit at Guy’s Hospital in 1986 reported by Harding (2003) revealed that patients with joint hypermobility found stretching helpful. This came as a surprise to the audit’s authors, but has been borne out repeatedly in clinical experience. Stiffness is a common complaint, with many hypermobiles saying they ‘feel like a 90-year-old’.” From Physiotherapy and occupational therapy in the hypermobile adult by Rosemary Keer & Katherine Butler 2010 Elsevier Ltd. DOI: 10.1016/B978-0-7020-3005-5.00013-6.
- — Ibid.
- — Jess Glenny, an experienced yoga teacher who lives with EDS suggests, “If you teach a yin style, be aware that for some hypermobile people an optimal yin stretch may be one to two minutes, and extending the hold time may result in damage to tissues. The appropriate duration will vary from person to person, and for the same person in different postures. Encourage students to track their own edge and emphasise that it is always OK to come out of a posture. The optimal hold time is not five minutes but when you feel ‘cooked’.”
 Enhanced ranges of motion due to an injury to a joint
Enhanced ranges of motion due to an injury to a joint